Click on a heading to expand the description for each item.
| a.c. | Take food ‘ante cibum’ Before food |
| b.d. | Take medicine ‘bis die’ Twice daily |
| o.d. | Take medicine ‘omni die’ Every day |
| o.m. | Take medicine ‘omni mane’ Every morning |
| o.n. | Take medicine ‘omni nocte Every night |
| p.c. | Take medicine ‘post cibum’ After food |
| p.r.n. | Take medicine ‘pro re nata’ When required |
| q.d.s | Take medicine ‘quarter die sumendum’ To be taken four times daily |
| q.q.h. | Take medicine ‘quarta quaque Every four hours |
| t.d.s. | Take medicine ‘ter die sumendum’ To be taken three times daily |
| t.i.d. | Take medicine ‘ter in die’ Three times daily |
Brief staring spells and a loss of consciousness lasting between 5 to 10 seconds. It is a generalised seizure often beginning in childhood. Recovery is immediate. Learn more about epilepsy types below.
These brief staring spells last longer and do not start or finish abruptly as the seizures mentioned above. They can be accompanied with other features such as slight head nodding or a chewing action. Learn more about epilepsy types below.
Will normally cover the cost of your injury as the result of your seizure. See the ACC website here for more information.
Claims helpline: 0800 101 996
This supplement is for people over 16 years of age who have accommodation costs and it is income-tested.
There are various devices for seizure alarms including; camera devices, EMFIT alarms, and fall detectors. Be aware that there are limitations to all alarms.
For more information see our article on 10 alarms that detect seizures.
If you are in need of an ambulance because of a seizure, please know that you will be billed for it unless you are a paid-up St John member. Unpaid bills will be forwarded to a debt collector and so please think about joining an ambulance service, such as St John. If you are on a benefit, you may be able to receive financial assistance to help you pay an annual subscription, under ‘Disability Allowance’.
Do not cure epilepsy but help control seizures. Some medications enhance particular chemical processes within the brain and others work by blocking or inhibiting them. See fact sheet #7 for more information on epilepsy and medication.
See also “medications commonly used in the treatment of epilepsy” under “M” and also side effects.
Can affect many people with epilepsy. Please see your GP or neurologist for help and they will put a plan of action in place for you. You may be prescribed antidepressants or be seen by a ‘talking therapist” and given cognitive behaviour therapy (CBT). Mindfulness, hypnotherapy, yoga, exercise and massage may also help with your mental health.
Free New Zealand based CBT courses are also available online at www.justathought.co.nz/courses
Is an illustrated book written and published by EWCT to help improve the quality of life for children living with epilepsy. Buy your copy here.
A brief loss of unconsciousness and a person’s muscles slacken and he/she may fall to the ground. Atonic seizures used to be called ‘drop attacks’. See our fact sheet on ‘epilepsy types‘ for more information.
Are focal-aware seizures that many see as a warning that a ‘bigger seizure event’ may happen. An aura can last several seconds, or minutes, and it can give people an opportunity to make themselves safe. Some people are unable to describe these ‘auras’ but many can experience things such as tingling/painful/electric shock or even numbness sensations. They may see flashing/ flickering lights or go temporarily blind. They may be able to smell unpleasant odours, experience acidic, bitter, salty, sweet or metallic tastes or have unusual gut sensations. Some people are able to hear voices or hallucinate.
Autoimmune epilepsy (AE) is caused by a change in the body’s immune function. AE often begins with seizures developing over days to weeks. People with cancer, a history of another autoimmune disease, or a parent, sibling or child with an autoimmune disease may be more likely to develop autoimmune epilepsy.
For more information please see the autoimmune article on epilepsy.com
Are repetitive movements that are found in focal seizures with awareness impairment (focal impaired awareness) and well as in some absence seizures.
The types of repetitive behaviours depends on the location of the seizure activity in the brain and, are generally found in the temporal and frontal lobes, although it is possible for automatism to appear in the parietal and occipital lobes.
Automatisms in the temporal lobes can include behaviours such as lip smacking, chewing, swallowing, fumbling, picking, grunting, screaming, undressing, repeating a word, repetitive tapping. Automatisms in the frontal lobes can include such behaviours as cycling movements, turning the head to one side, pelvic thrusting.
See our fact sheet on ‘epilepsy types‘ for more information.
Seizures can be hard to spot in babies. In this fact sheet you will discover the many seizure types and diagnoses.
Epilepsy Action in the UK have provided this handy page of information on the subject.
Find out which of the “Work and Income” (WINZ) benefits that you are entitled to: https://www.workandincome.govt.nz/online-services/index.html
https://www.workandincome.govt.nz/products/a-z-benefits/index.html
Phone: 0800 559 009 if you are under 65 years old
Phone: 0800 552 002 if you are over 65 years old
Work and Income managers do not necessarily understand epilepsy, and how it affects you, and so please take along an advocate to your appointments if you need help.
Is an illustrated book written and published by EWCT to help de-
mystify the epilepsy condition. Buy your own copy here.
Along with the spinal cord, makes up the human central nervous system. It controls our breathing, our beating heart, our ability to use our senses, how we receive and gather information, and even our behaviour and personality. The major parts of the brain consists of two halves (the left and right hemispheres) and each half is divided into four lobes (temporal, frontal, parietal and occipital). See fact sheet ‘The brain’ below for more information.
Epilepsy surgeries typically involve removing a small part of the brain that is responsible for generating seizures. Epilepsy surgery might also involve implanting a device in the brain that helps control seizures. See this link for further information.
There is no reason why women who have taken anti-epileptic medication throughout their pregnancy should not be encouraged to breastfeed their baby (Veiby 2013). However, women should be counselled on the signs of risk to be aware of, in particular excessive somnolence and poor weight gain. The risks increase with multiple drug regimens.
For more information see this booklet from breastfeeding-and-medication.co.uk
Various surveillance-specialty shops will tailor-make your audio and video requirements for monitoring loved ones with epilepsy. Information is sent to a smart phone via an app.
For an example see the SAMi™ device on this page.
Is an intensive care programme aimed at people with chronic health conditions, serious medical/mental health needs, or a terminal illness so that they may be more effectively managed by their health care team. To see if you are eligible please ask your GP.
Are seizures that occur around a woman’s menstruation cycle. http://www.epilepsy.com/information/professionals/refractory-seizures/potentially-remediable-causes/catamenial-epilepsy
There are many known causes of epilepsy:
- Genetic influences
- Medical disorders
- Head trauma
- Sports/car accidents
- Meningitis
- AIDS
- Developmental disorders
- Cerebral palsy, autism, Down syndrome
- Dementia
- Birth trauma
- Poisoning
- Lead/alcohol/drug
- Chemical and hormonal imbalance
- Autoimmune changes in body function
All of these are referred to as symptomatic epilepsy because the causes are known.
In most cases, there is no known cause (idiopathic) as to why a person has epilepsy but it would usually be genetic or inherited.
This allowance may be paid to the main carer of a child with a disability under the age of 18 years, if “the child has been assessed as needing constant care and attention for at least 12 months because of a serious disability’. This benefit is not income tested.
A comorbidity is a second disease or illness that happens alongside epilepsy. People with certain comorbidities are more likely to live shorter lives. Sadly, research shows that people with learning disabilities and epilepsy have a lower life expectancy.
Please develop a good relationship with your preferred GP and make the most of your 15-minute appointments. Be prepared. You are allowed to take someone to help you. Take along your EWCT seizure diary if needed.
- Take a list of your medications. Say if you are having problems with them.
- Make a list of your main health concerns.
- Have any questions answered to your satisfaction.
- Arrange a follow-up visit if needed.
Would you know what to do if someone is having a seizure?
Visit our fact sheet below for more information on what to do if someone is having a convulsive seizure,
Teach children what to do using these children’s fact sheets:
Chatterbox-puzzle.pdf
What to do if someone is having a seizure.pdf
Can be hazardous when you have epilepsy. Learn how to cook safely. For more information and advice see how fact sheet below.
Nationwide Counselling Services
1737 |
Free call or text to speak with a trained professional counsellor at any time of the day for callers seeking help with: anxiety, depression, suicidal thoughts orfeeling overwhelmed in life. |
|
Alcohol/Drug Helpline |
Assistance in information and support in drug and alcohol abuse. |
|
Anxiety New Zealand |
Callers are given support, treatment and education for children, adults and their families experiencing, anxiety, phobias or depression and other mental health issues |
|
Depression Helpline |
Talk to a trained counsellor for advice, information and support |
|
EAP Services |
Employee Assistance Programme- provides practical assistance to employees when personal or work issues affect their ability to do their job or impact on personal wellbeing. Issues may include:
Confidential counselling services are available throughout NZ and overseas. | |
Gambling Helpline |
24 hr freephone service that you can call to receive immediate support for gambling addiction - Completely anonymous. |
|
Kidsline |
New Zealand’s original telephone counselling service for all kids up to 18 years of age |
|
Lifeline |
Callers can talk to counsellors who are trained to deal with psychological and emotional distress, financial and work issues, marriage and family/whanau problems or abuse |
|
Rural Support Trust |
Have a confidential chat about you, your business, the weather, your finances; or a neighbour, partner, friend, family member, or worker. |
|
Salvation Army |
Supporting families and individuals in need with budgeting advice, food and clothing assistance and life skills programmes. |
|
Samaritans |
Confidential, |
|
SPARX |
SPARX is a computer program that helps young people with mild to moderate depression, anxiety or stress. It is based on a type of ‘talking therapy’ called cognitive behavioural therapy (CBT). |
|
Suicide Crisis Helpline |
A free, nationwide service available 24 hours a day, 7 days a week and is operated by highly trained and experienced telephone counsellors who have undergone advanced suicide prevention training. If you think you, or someone you know, may be thinking about suicide, call the Suicide Crisis Helpline for support. If you believe either you, or someone you know, is in immediate danger, please call emergency services immediately on 111. |
|
Supporting Families in Mental Illness |
Receive information and support for families/whanau |
|
The Lowdown |
Support and information for young people experiencing depression and anxiety |
|
Victim Support |
Victim Support provides a free, nationwide support service for people affected by crime, trauma, and suicide in New Zealand. Help is given to clients to find safety, healing, and justice after crime and other traumatic events. |
|
What’s Up |
0800 What’s Up is here for any child or teenager |
Youthline |
Mental Health and Addiction Service. Youthline works with young people. Their families and those supporting young people |
Call 111 for any emergency
Nationwide Counselling Services
1737 |
Free call or text to speak with a trained professional counsellor at any time of the day for callers seeking help with: anxiety, depression, suicidal thoughts orfeeling overwhelmed in life. |
|
Alcohol/Drug Helpline |
Assistance in information and support in drug and alcohol abuse. |
|
Anxiety New Zealand |
Callers are given support, treatment and education for children, adults and their families experiencing, anxiety, phobias or depression and other mental health issues |
|
Depression Helpline |
Talk to a trained counsellor for advice, information and support |
|
EAP Services |
Employee Assistance Programme- provides practical assistance to employees when personal or work issues affect their ability to do their job or impact on personal wellbeing. Issues may include:
Confidential counselling services are available throughout NZ and overseas. | |
Gambling Helpline |
24 hr freephone service that you can call to receive immediate support for gambling addiction - Completely anonymous. |
|
Kidsline |
New Zealand’s original telephone counselling service for all kids up to 18 years of age |
|
Lifeline |
Callers can talk to counsellors who are trained to deal with psychological and emotional distress, financial and work issues, marriage and family/whanau problems or abuse |
|
Rural Support Trust |
Have a confidential chat about you, your business, the weather, your finances; or a neighbour, partner, friend, family member, or worker. |
|
Salvation Army |
Supporting families and individuals in need with budgeting advice, food and clothing assistance and life skills programmes. |
|
Samaritans |
Confidential, |
|
SPARX |
SPARX is a computer program that helps young people with mild to moderate depression, anxiety or stress. It is based on a type of ‘talking therapy’ called cognitive behavioural therapy (CBT). |
|
Suicide Crisis Helpline |
A free, nationwide service available 24 hours a day, 7 days a week and is operated by highly trained and experienced telephone counsellors who have undergone advanced suicide prevention training. If you think you, or someone you know, may be thinking about suicide, call the Suicide Crisis Helpline for support. If you believe either you, or someone you know, is in immediate danger, please call emergency services immediately on 111. |
|
Supporting Families in Mental Illness |
Receive information and support for families/whanau |
|
The Lowdown |
Support and information for young people experiencing depression and anxiety |
|
Victim Support |
Victim Support provides a free, nationwide support service for people affected by crime, trauma, and suicide in New Zealand. Help is given to clients to find safety, healing, and justice after crime and other traumatic events. |
|
What’s Up |
0800 What’s Up is here for any child or teenager |
Youthline |
Mental Health and Addiction Service. Youthline works with young people. Their families and those supporting young people |
Call 111 for any emergency
This is when there is no known cause for the person’s epilepsy. Data vary, with some findings suggesting people may live around two years less. But other data (as noted above) suggests some people with cryptogenic epilepsy could live longer than the average.
Some people with focal-aware seizures can experience Déjà vu (feeling of being there before, but never have).
Are made by an epilepsy specialist. There is no test for epilepsy and doctors are partly reliant on eye witness accounts of what has been observed. See fact sheet #18 on Epilepsy diagnosis and treatment.
Covers certain types of costs
- alternative treatment
- ambulance fees and subscriptions
- authorised consumables
- clothing
- counselling
- day care for the elderly disabled
- gardening, lawns and outside window cleaning
- gym and swimming pool fees
- medical alarms
- medicAlert costs
- medical fees
- nicotine replacement products
- pharmaceutical charges
- power, gas and heating
- private paying patients
- rental equipment
- residential care services
- special foods
- telephone
- transport-counselling
- transport-disability
- transport- personal health
- vitamins, supplements, herbal remedies and minerals For more information see “Benefits”
In New Zealand all children have the right of enrolment at their local main-stream school. It is the role of the MOE to provide support for children with special needs by providing the following services.
Early intervention services
This service is available to a child from birth to school age by providing access to speech and language therapists, educational psychologists, educational support workers, deaf advisors, occupational therapists and physiotherapy.
For more information and contact details:
Phone: 0800 622 222
Email: special.education@mindu.govt.nz
Web: www.education.govt.nz
Ongoing Resourcing Scheme (ORS)
This is available to children who have high or very high health needs and must have: extreme or severe difficulty with either learning, hearing, seeing, moving about or using language and social communication, or a combination or moderate-to-high difficulty with learning plus any two of the above difficulties at the moderate level.
ORS funding may help pay for teacher aid time, resources for the classroom and specialist services such as OTs, physiotherapy, educational psychologists, behaviour support and assistance technology (such as hearing devises, specialised seating and computer aids).
For more information and contact details
Phone: 0800 622 222
Email: special.education@mindu.govt.nz
Web: www.education.govt.nz
Resource Teacher of Learning and Behaviour (RTLB)
An RTLB teacher supports students who experience learning barriers and assists teachers and schools to better assist these individuals.
For more information and contact details:
Phone: 0800 622 222
Email: special.education@mindu.govt.nz
Web: www.education.govt.nz
Special Education Grant (SEG)
Most New Zealand schools receive these small grants dependent on the school’s size and decile rating. These grants can be used to support all types of students.
Special schools
If your child has high, or very high needs another option may be a Special School. There are 28 day schools and 6 residential homes throughout New Zealand.
http://www.education.govt.nz/search/SearchForm?Search=special+schools&action_results=Go
Special Education Needs Coordinator (SENCO)
An experienced teacher usually holds this role and is involved in the development of the ‘individual education plan’ (IEP). The SENCO will also assess the needs of a child as well as coordinating appropriate resources, supports and services.
In New Zealand the MOH funds a range of supports for people with disabilities generally up to 65 years of age, to help them live an everyday life in their communities. A person must be eligible to receive these support services and have a physical, intellectual or sensory disability (or a combination of these) which:
- Is likely to continue for at least six months
- Limits their ability to function independently, to the extent that ongoing support is required.
The MOH will not cover:
- A disability resulting from an accident such as paraplegia or brain injury, ACC will administer all supports for that person.
- Chronic health conditions, such as schizophrenia or depression, asthma and diabetes. District Health Boards (DHBs) funds some supports here. DHBs also support people with ageing conditions such as Alzheimer’s.
For more information regarding eligibility please go to:
www.health.govt.nz/your-health/services-and-support/disability-services
Email: disability@moh.govt.nz
Phone: 0800 373 664 (Monday to Fridays, 8am-5pm)
Types of MOH support available
- Home and community support (e.g. household management or help, personal care)
- Equipment and Modification Services (e.g. funding for equipment such as wheelchairs; home modifications such as ramps and widened doorways; and vehicle modifications such as a hoist)
- Hearing and Vision Services (e.g. hearing aids; children’s spectacle subsidy)
- Respite and carer support
- Community and residential support
- Supported living
- Behaviour support (Autism Spectrum Disorder, ASD Communication and Behaviour Support, ASD Plus Parent education)
- Child Development Services, which are based in DHBs. Referrals are made by a GP, paediatrician or nurse.
- Individualised Funding (IF) which gives families greater choice and control over their household management and personal care funding.
For more information regarding eligibility please go to:
www.health.govt.nz/your-health/services-and-support/disability-services
Email: disability@moh.govt.nz
Phone: 0800 373 664 (Monday to Fridays, 8am-5pm)
These seizures involve the mind, rather than the body, and can be difficult to diagnose. Treatment involves psychiatric or psychological support.
See our fact sheet on “understanding seizure disorders” for more information.
There are risks associated with driving whilst having epilepsy. If you have epilepsy you may also be excluded from driving a mobility scooter and battery- powered wheelchair. You will need to seek advice from your GP or neurologist.
See our ‘driving and epilepsy’ fact sheet below.
Even though medicine is legal, it can affect your cognitive processing, reaction times and perception of reality. It can also make you more fatigued. It’s illegal to drive when impaired by any medication. This is because you risk causing death or serious injury to yourself and other people.
Disability Support Link is an assessment and service coordination service that assists in obtaining home support services for people with disabilities in the Waikato, King Country, Thames Valley and Peninsula and may include:
- Household assistance
- Personal care
- Day programmes (non-therapeutic)
- Carer support
- Residential care and support
- Referral to other services
Referrals can be made by clients, their family/whanau, GPs, a health professional, disability groups/organisations or a friend.
For more information, please phone:
Hamilton are (07) 839 1441 or 0800 55 33 99
Is a fundamental human right and students cannot be excluded or treated less favourably because of epilepsy. See the ‘how to help a student with epilepsy‘ fact sheet below.
Your child may be eligible to assistance whilst at school. Please ask about ‘High Needs funding’.
(electroencephalograph) is used as a diagnostic tool which measures brain activity.
Small electrodes are placed on the person’s head with a sticky paste and the computer records electrical activity occurring in the brain. See Kieran’s EEG story for:
Embrace is the first medical quality wearable to help measure stress, epileptic seizures, activity and sleep. As well as identifying seizures it also has a feature to notify parents and caregivers when a seizure occurs.
“When people that have Epilepsy wear Embrace, they will get an alert when an unusual event happens, like a convulsive seizure. It will go via their smartphone to parents, roommates.”
For fire, police and ambulance Show children how to dial the emergency number (How-to-dial-111-for-an- ambulance.pdf)
Is designed for monitoring and detecting seizures with muscle jerking of a sleeping person with epilepsy. Available in New Zealand through reidtechnology.co.nz
On many job application forms you are asked to disclose if you have a disability or health condition that could affect your ability to work. If there is no specific question on the application form, then there is not necessarily any need to reveal it.
Most people with epilepsy (at least 70%) are well controlled with medications and they work in a wide variety of jobs where their epilepsy does not impact on their safety or the safety of others.
Do your own research about a job that potentially suits your qualities, your qualifications, interests and skills, and at the same time consider your epilepsy condition. Complete the “careers quest quiz” if you need inspiration in choosing a career.
Some jobs have known occupational hazards that would pose even greater risks to people with epilepsy, and you would automatically be barred from applying for them.
Use your common sense when applying for jobs. Be positive and seek help in finding employment. Most people find jobs through word of mouth and so you need to sell yourself. You could try organisations such as Workbridge or Enrich Plus that help people with disabilities find employment.
If you have not disclosed that you have epilepsy, it may nevertheless be useful to do so just in case you have a seizure at work. Let your colleagues know what sort of seizures you have and devise an action plan so that everyone knows how to help you should you have one. You may need to have a conversation with your boss to discuss why you need some time off now and then for a neurology appointment or to recover from a seizure. It is about being reasonable and fair.
Employers and employees are governed by the “Health and Safety in Employment” Act and reasonable care must be taken to ensure everyone’s safety, including yours.
Is a neurological condition caused by a burst of abnormal activity in the brain causing seizures. Seizures generally lasts for a brief period of time and result in an alteration in sensation, behaviour and consciousness. There are over 40 different seizure types and many ways in which they are presented. Seizures can be described as ‘generalised’ or ‘focal’. See the ‘what is epilepsy‘ fact sheet for more information.
See your EWCT epilepsy advisor who will help develop a personalised epilepsy action plan for you.
For EWCT is in November and is advertised through our webpage. You will find a calendar of epilepsy facts and a list of famous people who have (or had) epilepsy. Please get behind EWCT and help to break down the epilepsy stigma.
Book your epilepsy awareness seminar with your EWCT epilepsy adviser maria@ewct.org.nz or info@ewct.org.nz
There are at least 40 seizure types and it is regarded as a spectrum of disorders. See the ‘epilepsy types‘ fact sheet for more information.
Gives advice, support and information. See ‘what we offer‘ for more information.
Is useful for those who fall during a seizure. If a fall occurs, the intelligent sensors within the detector analyse the event for 20 seconds. After 20 seconds, it lights up and emits warning tones, indicating that an alarm call is about to be place. At this point any accidental activation can easily be cancelled by the wearer at the press of the cancel button.
There is a help button that can be pressed at any time for assistance. This will connect you with Bupa’s response team, who will get you the help you need, and stay in touch until they know that you are safe.
For more information please contact:
Bupa Medical Alarms 0800 60 80 99 or www.bupa.co.nz
“There have always been people with epilepsy. Since the dawn of time, epilepsy has affected millions of people from beggars to kings. It is one of the oldest conditions of the human race”. You will discover some names of famous people are who have lived with, or live with, epilepsy by completing our word-find.
Is intense electrical activity that occurs in an area on one side of the brain. What these seizures look like depends on which area of the brain is affected. See the ‘epilepsy types‘ fact sheet for more information.
Some anti-epileptic medications, such as Epilim, may affect the unborn baby. For more information please see: http://www.facsnz.com/about/
Occur on both sides (hemispheres) of the brain and they result in a degree of unconsciousness. There are various generalised seizures: tonic, atonic, myoclonic, tonic clonic, typical and atypical absence seizures.
Here are some very useful methods to help you help your child or baby take their regular medicine.
healthify.nz – giving medicines to children and babies
This is a New Zealand site and the information is available in multiple languages and in video format as well.
Your GP (doctor) will take responsibility for your epilepsy condition with regard to prescribing your medications, making sure that your seizures are under control, and that you are feeling well.
http://www.health.govt.nz/your-health/services-and-support/health-care-services/visiting-doctor
If your epilepsy is under control, and you need support to improve your general health and wellbeing, then an Active & Well Green Prescription may help you.
An Active & Well Green Prescription is a free 3 month coaching and support service to help you lead a more active and healthy lifestyle. Anyone who is not doing 30 minutes of moderate activity five days a week is eligible. The Green Prescription programme is a Ministry of Health funded service.
Visit the online referral form below to register:
http://www.sportwaikato.org.nz/programmes/active-and-well/green-prescription.aspx
Is not a medical record but it gives information about the things that are important to you for when you are receiving hospital care. Ask for your health passport from the Health and Disability Commissioner.
Email: healthpassport@hdc.org.nz or
Phone: 0800 111 2233
Website: www.hdc.org.nz
Is a free 24 hour/day health and medical advice service. Please phone 0800 611 116 to speak to a specialised Healthline nurse.
Are you concerned about the health care that you have received?
You can speak to an independent person about your options:
Freephone 0800 801 482 or
Cary Douglas (07) 850 5744 (Hamilton)
Margaret Southgate (07) 856 9522 (Hamilton)
Ruth Strawbridge (07) 210 1258 (Cambridge)
Gwen Roberts (07) 886 9594 (Tokoroa)
Lorraine Edwards (07) 896 8754 (Taumarunui)
You may wish to write to:
Health Consumer Services
PO Box 15019
Dinsdale
Hamilton 3243
St John, in Hamilton, offers a free community service that transports people to essential medical and health-related appointments, and then takes them home again. There is no charge for the shuttle transport, but a donation is appreciated to cover costs. St John does not offer this service in all areas.
To find out more about St John Health Shuttle, or to book a journey, call toll free on 0800 000 606
Health Transport Services in the Region:
Coromandel
Coromandel Independent Living Trust
Tiki House
45 Tiki Rd
(07) 866 8358
Kawhia
Ngati Maniapoto Marae Pact Trust
(07) 878 6234
Matamata
NZ Red Cross
Te Rapa Rd
Hamilton
(07) 849 0285 -press the extension for the Waikato Services Centre
Matamata Community Health Shuttle
(07) 888 6040 or at
Matamata Citizen’s Advice Bureau
Railside by the Green.
41a Hetana Str
Morrinsville
NZ Red Cross
Te Rapa Rd
Hamilton
(07) 849 0285 -press the extension for the Waikato Services Centre
Otorohanga
NZ Red Cross
Te Rapa Rd
Hamilton
(07) 849 0285 -press the extension for the Waikato Services Centre
Paeroa
Paeroa Community Support Trust
Cnr Mackie and Willoughby Streets
Paeroa
(07) 862 6110
Putaruru
Tokoroa Hospital Reception
(07) 886 7239
New Zealand Red Cross
Te Rapa Rd
Hamilton
(07) 849 0285 -press the extension for the Waikato Services Centre
Raglan
Raglan Community House Society
Bow Street
Raglan
(07) 825 8142
Tairua
Tairua Care and Friendship Club
(07) 864 9550
Taumarunui
Taumarunui Kokiri Community Trust
(07) 895 5919
Taumarunui bus
Waikato Hospital co-ordinates this transport
(07) 838 8899 ext 96125 (enquiries desk)
Te Aroha
New Zealand Red Cross
Te Rapa Rd
Hamilton
(07) 849 0285 -press the extension for the Waikato Services Centre
Te Awamutu
Taumarunui bus
Waikato Hospital co-ordinates this transport
(07) 838 8899 ext 96125 (enquiries desk)
Or try Red Cross
Te Rapa Rd
Hamilton
(07) 849 0285 -press the extension for the Waikato Services Centre
Te Kauwhata
Rural Women NZ -Te Kauwhatu
(07) 826 3980
Te Kuiti
Taumarunui bus
Waikato Hospital co-ordinates this transport
(07) 838 8899 ext 96125 (enquiries desk)
Thames
Te Korowai Haurora o Hauraki
210 Richmond Street
Thames
(07) 868 5375
Tokoroa
Tokoroa Hospital reception
(07) 886 7239
Waharoa
New Zealand Red Cross
Te Rapa Rd
Hamilton
(07) 849 0285 -press the extension for the Waikato Services Centre
Waihi
The Order of St John
Johnston Street
Waihi
(07) 863 8666
Whangamata
Whangamata Community Services Trust
101 Casement Rd
Whangamata
(07) 865 7065
Whitianga
Whitianga Community Services Trust
2 Cook Drive
Whitianga
(07) 866 4476
Supports students who have health needs as a result of a significant health condition and who would need care for more than 6 weeks. The fund does not cover seizures that occur infrequently, or in clusters, with long seizure-free periods. The fund, however, will cover a student with supervision around medication, toileting/showering, playtime activities and anything requiring support in swimming, science and technology.
More information can be found on the education.govt.nz website here.
Bracelets, necklaces and wallet cards improve the safety and medical care of a person with epilepsy in public. You can view a list of options at:
- Medic Alert (ongoing membership cost)
- Mediband (no ongoing costs)
- MyIdentity (no ongoing costs)
Note that MyIdentity currently provides a special discount for members of EWCT and our clients. Please contact us for more information if you are interested.
This is when the person’s seizures are likely caused by their genes. These people have a slightly lower life expectancy than the average – around two years.
International League Against Epilepsy https://www.ilae.org/
Are those seizures that mimic epileptic ones such as in febrile convulsions, fainting, mini strokes, sleep disorders, movement disorders, panic attacks, psychogenic and low blood sugar seizures. These ‘imitators’ can lead a doctor in making a wrong diagnosis of epilepsy.
- Supported Living payment
- Child Disability Allowance
- Disability Allowance
- Childcare subsidy
- Working for Families Tax Credits
- Accommodation Supplement
- Assistance for Hardship
- Community Services Card
- Supported Living Payment
- Sickness benefit
- Disability allowance
- Assistance for hardship
- Accommodation supplement
- Community services card
Some people during a focal-aware seizure can experience Jamais vu (a feeling that something is very familiar but it isn’t)
Are available from Workbridge to assist people with disabilities in New Zealand to enable them to participate in open employment. The funds include: job support, training support and self− start. Please discuss your options with a Workbridge staff member: 0508 858 858
The ketogenic diet is a rigid, mathematically calculated, doctor-supervised diet, which alters the body’s chemistry by simulating the metabolism of a fasting body. It is a diet high in fat and low in protein and carbohydrate and is formulated to sustain the state of ketosis within the body.
When a child starts the diet the ratio of fat to protein and carbohydrate combined are usually set at 4:1. Approximately 90% of total calories are derived from fat, usually in the form of butter, oil or cream.
When reserves of glucose are depleted (for example, though fasting), the body can no longer use glucose to give it energy. This forces the body into a state of ketosis, burning fat quicker than it can be completely used, which results in a residue of ketones to build up in the blood, spilling over into the urine. When these ketones build up, they act as a kind of sedative, preventing the sudden disturbances in the electrical functioning of the brain that lead to seizure activity. For the diet to be successful, a child’s body must be in a constant state of ketosis.”
Named after the ketone bodies excreted in the urine during ketosis, the ketogenic diet has been around since the 1920s. It was originally developed at the Mayo Clinic and Johns Hopkins University Hospital (Baltimore, USA) but as anticonvulsants came onto the market in the 1940s and 1950s, the ketogenic diet fell into disuse.
The diet is usually started in hospital, under the supervision of a neurologist, and is devised individually by a trained dietitian to fit the age, height, weight and metabolism of each child. Calculating the ketogenic diet is three parts science and one part art. The art part is a combination of common sense, empathy, and intuition. There is no promise that the diet will be easy initially, but if it works – if it works – it becomes not only tolerable, but absolutely amazing.
Please note that the ketogenic diet also shows promise for treating Alzheimer’s, Parkinson’s, autism, depression, migraines and cancer.
Credit:
The Daisy Garland
See our page on Ketogenic diet therapies for adults with epilepsy for more information.
Here is the exceptional circumstances application form for funding of an alternative brand of lamtrogine.
 Life Tube is a small plastic tube which contains important health information that can be used in an emergency by the Police, Ambulance, Fire Service or anyone else who might be on hand.
Life Tube is a small plastic tube which contains important health information that can be used in an emergency by the Police, Ambulance, Fire Service or anyone else who might be on hand.
If you have an accident at home and are either in shock or unconscious, you may not be able to tell the emergency services about your medication which could delay treatment at hospital. The Life Tube can do the talking for you.
Inside the tube there is a single sheet of paper which you fill out on both sides with all the relevant details of your medication and the contact details of your Doctor, next of kin, pharmacist etc. There is also space to write down any allergies and known health conditions you may have. The tube contains a large red sticker which we recommend you stick on front of your fridge to alert emergency services that you have a Life Tube in there. The kitchen and the fridge are easy places for emergency services to access.
When you purchase a Life Tube we recommend the following:
- Complete your details as soon as possible
- Update your details throughout the year as things change
- Ask your pharmacy for a print-out of your medication to pop into the Life Tube but make sure there is a date on it
Life Tubes are available for sale at Age Concern Hamilton for just $5…it could save your life.
Find PEACE and become a member of EWCT.
See our fact sheet on living with the challenges of epilepsy below.
Medicine Management Service is a free service to help people get the best from their medicines. A qualified pharmacist will arrange a 40-50 minute appointment to discuss:
- Medicines and why we take them
- How medicines work in the body
- How to take medicines correctly and at the best times
- How to get the most out of medicines
The pharmacist will raise any issues or concerns with the patient’s doctor as needed.
The Waikato mobile pharmacist is Rachel Bell (027) 268 5704 rachel@midcpg.co.nz
To learn more about these services please go to: www.midcpg.co.nz
Carbamazepine (Tegretol)
Clobazam
Clonazepam
Ethosuximide (Zarontin)
Gabapentine (Neurontin)
Lamotrigine (Lamictal)
Leviteracetam (Keppra)
Nitrazepam (Nitepam, Mogadon, Insoma 5, Nitraclos)
Oxcarbazepine (Trileptal)
Phenytoin (Dilantin)
Primidone (Mysoline)
Sodium Valporate (Epilim)
Tiagabine (Gabitril)
Topirimate (Topamax)
Vigabitrin (Sabril)
All AEDs have a list of possible side effects. “Start low and go slow” helps to minimize the effect of AEDs on your body. Please watch for:
- Behavioural changes (especially in children), irritability, mood changes, drooling
- Memory issues
- Gum swelling, acne, increased body hair, weight gain, weight loss
- Dizziness, double vision, insomnia, headaches, drowsiness, nausea
- Pins and needles feeling of hands and feet
- Rashes
See our fact sheet on ‘epilepsy and medication‘ for more information.
Is responsible for the regulation of medicines and medical devices and ensure that medicines and medical devices are acceptably safe. You can find information about the medications that you are taking at medsafe.govt.nz.
Is challenging for most people at some point in their lives, and for people with epilepsy, it is not unusual. Memory loss can occur because of seizure activity within the brain, which disrupts memory processes, and sometimes because of the use of antiepileptic drugs (AEDs) which can cause drowsiness or attention problems.
Visit fact sheet ‘epilepsy and memory‘ for more information.
Midazolam belongs to a group of medicines called benzodiazepines. It can be used in a number of conditions but in this case midazolam is used for treating seizures (fits) in an emergency.
Here is a video on how to administer Midazolam:
For more information about Midazolam view the leaftlet:
- Basic audio-visual equipment. Some seizures may be silent and can therefore be missed with baby monitors.
- Monitors that detect movements. A special sensor pad to detect movements associated with seizures can be used to alert and send messages to caregivers. An example would be the “Emfit Epileptic Tonic-Clonic Seizure Monitor”.
- Multi-symptom monitoring for detecting symptoms associated with seizures including bed-wetting and salivation. Eg. SAMi™
- Monitors that detect changes in heart rate such as the Embrace smart watch.
You will find helpful tips as a mother with epilepsy here:
(magnetic resonance imaging): uses magnetic fields to detect structural abnormalities in the brain such as tumours and scar tissue.)
literally means muscle jerks.
How to use nasal Midazolam
Place the person in the recovery position or in the best position to allow easy administration of intranasal midazolam

- Twist off cap of the plastic midazolam vial
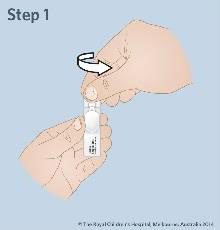
- Attach the syringe to the vial. Make sure that the syringe is upright. Withdraw the dose as prescribed. Push out any big air bubbles. Remove the ampoule from the syringe.
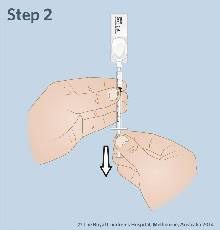
- Attach the syringe to the mucosal atomization device.
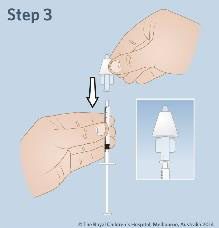
- Insert the mucosal atomization device loosely into a nostril and press the plunger quickly to give half of the dose. Remove the device and insert into the other nostril to give the remaining dose.
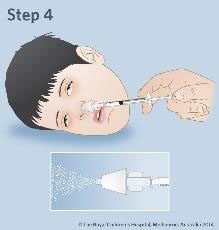
Phone the ambulance if the seizure has not stopped within 5 minutes or the person has laboured breathing.
In some cases, a second dose of midazolam can be given after 5 minutes.
Treats disorders that affect the brain, spinal cord, and nerves; neurologists do not perform surgery, that is done by a neurosurgeon. A neurologist will be involved in the diagnosing and treatment of epilepsy.
Is a specially trained psychologist who understand the relationship between the physical brain and behaviour.
Are often described as pseudo-seizures. They have a different cause but they can look similar to epilepsy and can affect people in similar ways. NES are not the result of a disruption of electrical activity in the brain.
Of what you see, when someone is having a seizure, helps with a diagnosis and classification of epilepsy and hence possible treatment. You may find the table in “recording seizures’ helpful in describing them. Using a camera or mobile phone as part of your observation also helps the neurologist in reaching a diagnosis.
It’s possible to renew subscriptions online. See this PDF guide on how to do this through the Zoom Pharmacy and Pharmacy Direct websites.
Helps a student join in and learn alongside other students at school. Once a student is in ORS, their funding stays with them throughout their time at school. Around 1 percent of students receive this support at any one time.
Is a specially trained doctor who manages the health and wellbeing of children.
Is a nationwide support and information service. Free phone 0508 236 236 or parenttoparent.org.nz
Are important people in your epilepsy care team. They prepare your medications and provide free, confidential and professional advice about your anti-epileptic medication.
They will discuss possible side effects, how to take your medication properly, and possible interactions with other medicines such as the contraceptive pill, alcohol, recreational drugs or natural therapies that you may be taking. Do not adjust or stop taking your medications except on the advice of your epilepsy specialist. Make sure that you never run out of your medications. Plan around public holidays and travel.
If you intend travelling, take enough medications for your trip and a copy of your prescription. Seek advice from your pharmacist should you be taking an overseas trip. See our fact sheet on epilepsy medication for more information. Visit Fact sheet 7 for more information on epilepsy medication.
Pre-ictal (prodrome)
This can last for hours or days before the ictal stage of a seizure. Not all people experience this.
Common symptoms are:
- Behavioural changes
- Cognitive disturbances
- Anxiety and mood changes
- Fatigue
- Sleep disturbances
- Speech disturbances
- Dysthymia, which is a milder, but long-lasting form of depression
- Headaches
- Changes in appetite
Ictal
This is the time from the first symptom to the end of the seizure activity. It is during this time that intense electrical activity is occurring in the brain. Symptoms that can occur during the ictal phase of a seizure may include:
- Rhythmic shaking and jerking of one arm or leg
- Shaking or jerking of the whole body
- tiffness of part of the body or the whole body
- Twitching of your face
- Tongue smacking
- Eye blinking
- Grunting noises
- Staring into space
- Sudden falling
- Dropping an object (due to altered consciousness or abnormal movement)
- Loss of bowel or bladder control
You can experience any combination of these symptoms during the ictal phase of a seizure, and you might not be able to remember the episode.
Post-ictal
The postictal phase refers to the period of time immediately following a seizure. The postictal phase can last for only a few seconds, several minutes or even days.
It is commonly thought of as the time during which the brain recovers from a seizure.
In the postictal state common symptoms are:
- Confusion
- Lack of conscious
- Tired
- Loss of bladder or bowel control
- Fear/anxiety
- Shame/embarrassment
- Thirsty
- Sore muscles
- Weakness
- Injuries
- Memory loss (duration of time varies)
- Sleepy
- General feeling of being “off” or “out of sorts”
Some people have uncontrollable violence. This can be shown in hitting or kicking. This is an uncontrollable reflex and a person means no harm.
Affects about 3% of the population and is more commonly found in children and adolescents than in adults. Seizures are triggered by flashing lights or certain visual patterns.
Each prescription is charged at $5. You become eligible for the subsidy once you have paid for 20 new prescription medicine items from 1 February each year. Ask your pharmacist if you qualify for the subsidy. Visit this page on health.govt.nz for more information.
Refers to an observed change in mood or behaviour in a person with epilepsy, hours or days before a seizure happens. Behaviours can include feeling angry, irritable or anxious.
For more information about Hamilton’s bus timetable, bus routes and fares, please go onto http://www.busit.co.nz/Hamilton-routes/ Seek out small town transport providers at your local Citizen’s Advice Bureau (CAB) or information centre, if you live outside of Hamilton.
Pregnancies should be planned, at least a year in advance, as this enables the neurologists to review your anti-epileptic medication. Some AEDs can affect the development of the unborn baby and so specialist advice and support are essential at least 3-6 months before starting a family. Most babies are born healthy to mothers who are taking AEDs.
AEDs affect your body’s ability to absorb folic acid and so it is advisable that you take higher-than-usual doses to prevent nervous system defects such as spina bifida in your developing baby. Iodine supplements are also recommended. Your specialist will prescribe an AED that gives you best seizure control whilst protecting your baby from its side effects. Any risks will be kept to a minimum. The effect of being pregnant is unpredictable in all women. Some may experience an increase in their seizures whilst others can have a decrease.
Here is a useful vocabulary list to explain what happens during a seizure. You may find this useful when describing your seizures. What do they look like?
| Awareness | Facial expressions | Head movements | Body stiffens | Jerking | Automatic movements | Speech |
|---|---|---|---|---|---|---|
| Fully aware | Staring | Sudden head drop | Whole body (If just one side, note which side) | Whole body | Hands clapping/ rubbing |
Able to talk normally |
| Confused | Twitching | Turns to one side (note which side head turns to) | Legs | Legs | Lip smacking/ chewing |
Unable to talk |
| Responds to voice |
Eyes rolling | Turns side-to-side | Arms | Arms | Walking/ wandering |
Incoherent/ nonsense words |
| Responds to light touch | Eyes blinking | Running | Mixing up words | |||
| Not responsive | ||||||
| Loss of consciousness yes/no | ||||||
| Incontinence yes/no | Bowel motion yes/no | |||||
The welfare and safety of all children in a school are paramount and so a number of factors need to be considered in developing risk management plans for individuals with epilepsy.
For more information visit the ‘risk management planning for teachers‘ fact sheet below.
SAMi™ is a sleep activity monitor for anyone (caregivers and individuals) who needs to watch carefully for unusual movements at night. During sleep, audio-video information from a remote infrared video camera is sent to an app that runs on an iOS device such as an iPhone or iPod Touch. The SAMi app records and analyzes the video for unusual activity. When an unusual event is detected, it sounds an alarm and records live audio and video from the SAMi network camera. Within seconds, the individual or caregiver can take any necessary action.
The home is the most common place for seizure-related accidents, followed by in the street and workplace. For more information see our fact sheet on ‘safety in the home‘:
Is an important tool to manage, record and keep track of seizures and epilepsy. It can be used to keep track of medications, side effects, seizure frequency and for help in identifying potential triggers.
Please contact Maria on maria@ewct.org.nz if you would like to receive a free copy.
Is the level of brain stimulation in which a person has genetically been programmed to have a seizure. A person with epilepsy has a lower-than-normal seizure threshold and therefore his/her brain is less resistant to seizures.
Are events or situations that can lower the seizure threshold and make a person more vulnerable to seizures. If you learn which things may trigger your seizures, then you and your GP can learn to manage your epilepsy more effectively.
Get a free copy of a seizure diary from your EWCT epilepsy advisor to help you to record your seizures. Some common seizure triggers include missed medications or medication change, tiredness or sleep deprivation, stress, alcohol and recreational drug use, feeling unwell and menstrual periods in women.
Below is a comprehensive list of different types of seizures. For more information and a general overview of seizures see our fact sheet on epilepsy types.
1. Absence Seizure (“Petit Mal”)
Absence seizures account for 2-4 percent of epilepsy. They are characterized by brief episodes of staring, usually lasting only 2-10 seconds and may happen repeatedly during the day. There is no warning before a seizure and the person is completely alert afterwards, with no memory of it. Because they are so mild, you might not even realize you had one and it’s easily not noticed by those around you.
2. Aicardi Syndrome
A rare inherited (genetic) disorder in which the structure that connects the two sides of the brain (corpus callosum) is partly or completely missing.
3. Alice in Wonderland Syndrome (Micropsia)
Children with Alice in Wonderland Syndrome (or AIWS) feel that their body is changing, because of migraines and headaches. They don’t just see themselves changing in size, though, but they also see other people, animals and objects look larger or smaller than they actually are. They can also feel that their hearing and sense of touch have changed. Like what happens to Alice in the beginning of the book, some people with epilepsy who also have AIWS can feel like they are falling down a hole…
Children are the most affected by Alice in Wonderland Syndrome. Most of the effects occur in the dark, where they feel the most scared. Oddly enough, some cough syrup ingredients might cause AIWS. Other causes for AIWS in children are Epstein-Barr Virus and Mononucleosis (or Mono for short). Most times, the symptom will last for only one month. And although it’s unlikely, adults are able to get Alice in Wonderland Syndrome as well.
4. Atonic Seizures (Drop Attacks)
Without warning, a person will abruptly loses consciousness, collapse and fall to the floor. Your head may drop suddenly, your eyelids may droop, your head may nod, and you may drop things. This is caused by sudden loss of muscle tone. Although it’s not usually associated with loss of consciousness and There is no convulsion, it’s possible to bang your head as you fall. Recovery occurs after a few seconds. You regain consciousness, and can again stand and walk.
5. Atypical Absence Seizures
The person will stare (as they would in any absence seizure) but often is somewhat responsive. You may experience eye blinking or slight jerking movements of the lips.
6. Autonomic Seizures
These seizures are accompanied by autonomic symptoms or signs, such as abdominal discomfort or nausea which may rise into the throat (epigastric rising), stomach pain, the rumbling sounds of gas moving in the intestines belching, flatulence and vomiting. This has sometimes been referred to as abdominal epilepsy. Other symptoms may include pallor, flushing, sweating, hair standing on end, dilation of the pupils, alterations in heart rate and respiration, and urination. A few people may experience sexual arousal, penile erection, and orgasm.
7. Benign Rolandic Epilepsy (Sylvan Seizures or Benign Partial Epilepsy of Children)
Accounts for more than one-third of epilepsy beginning in middle childhood between ages 3 and 13. Seizures usually occur infrequently in children, as generalized nocturnal seizures characterized by a variety of minor tonic-clonic movements and often affect only one side of the face. A typical attack involves twitching, numbness, or tingling of the child’s face or tongue (a partial seizure), which often interferes with speech and may cause drooling There’s a jerking of the corner of the mouth that may spread to the rest of that side of the face, causing a twisting motion. The child usually does not lose consciousness, except in cases of secondarily generalized seizures of this type. In rare cases, the seizure may progress to encompass the entire side of the body, becoming a generalized tonic-clonic condition. Seizures typically occur at night and these children are otherwise normal and healthy. The prognosis is favorable with 95% of children outgrowing their seizures by age 15.
8. Catamenial Seizures
This is seizure activity associated with a woman’s menstrual cycle. Studies have shown that fluctuations in female hormones prior to and during menstruation may elevate seizure frequency in some women. In a small percentage of women, catamenial seizures may occur only during the days just before their periods; for others, during the period itself. Higher ratios of estrogen to progesterone may increase seizure frequency. Water retention, electrolyte imbalance, and even poor sleep are also contributing causes.
The connection between menstruation and seizures has been demonstrated in women with simple partial, complex partial, and generalized tonic-clonic seizures. However, different types of seizures may be associated with different phases of a woman’s menstrual cycle. For example, a women with absence seizures may have more seizures during days 16 to 28 of her average cycle and may have the least during her period. A women with partial seizures, on the other hand, tends to have fewer seizures during days 16 to 28 and more just prior to ovulation and during menstruation.
9. Clonic Seizures
During a clonic seizure, you may lose control of bodily functions and begin jerking rhythmically in various parts of your body. Consciousness may be temporarily lost and followed by confusion. Clonic seizures begin in early childhood. With time, clonic seizures may eventually progress to generalized tonic-clonic seizures.
10. Complex Partial Seizures (Psychomotor or Temporal Lobe Seizures)
Begins with a blank look or empty stare. You may be unaware of your surroundings and seem dazed and confused. The seizure may progress to include chewing movements, mumbling, uncoordinated activity, or sometimes performing meaningless bits of behavior which appear random and clumsy. These may include picking at your clothes, trying to remove them, walking about aimlessly, picking up things, or mumbling. Someone experiencing a complex partial seizure may become frightened and try to run and struggle. Following the seizure, there will be no memory of it. A complex partial seizure usually lasts about 2 to 4 minutes. It may be followed by a longer lasting confusion. Once the pattern of seizures is established, it will usually be repeated with each subsequent seizure.
11. Dravet Syndrome — Severe Myoclonic Epilepsy of Infancy
(SMEI), is a severe form of epilepsy. It appears during the first year of life with frequent febrile seizures – fever-related seizures that, by definition, are rare beyond age 5.
Later, other types of seizures typically arise, including myoclonus (involuntary muscle spasms). Status epilepticus – a state of continuous seizure requiring emergency medical care – also may occur.
Children with Dravet syndrome typically experience poor development of language and motor skills, hyperactivity, and difficulty relating to others.
In 30 to 80 percent of cases, Dravet syndrome is caused by defects in a gene required for the proper function of brain cells.
12. Eclampsia
Convulsions are the other most common feature of this syndrome. Convulsions are usually generalized tonic-clonic in nature. Usually a brief single seizure occurs. Multiple seizures can also occur and status epilepticus is rare. Partial seizures or complex partial seizures can also occur. The seizures can occur prepartum, intrapartum, or postpartum. If the seizure occurs postpartum, it usually occurs within the first 24 hours after delivery, however, late postpartum eclamptic convulsions are by no means rare and have been reported as late as 23 days postpartum.
13. Ecstatic Seizures
Also called Dostoyevsky’s Epilepsy, are a type of seizure activity that is characterized by feelings of ecstasy or transcendent joy. Mystical, spiritual, and hallucinatory experiences often occur as well. The temporal lobe is effected by the seizure activity and provides a neural basis for these experiences. These seizures can involve more than one seizure symptom, such as tonic-clonic, tonic & more.
14. Febrile Seizures
Children aged 3 months to 5 years may have febrile seizures when they have a high fever. This occurs in only 2% to 5% of all children. A febrile seizure is usually mild and brief, often resulting in a slight slumping and loss of consciousness, or a rolling of the eyes back in the head. Sometimes there may be convulsive stiffening and jerking, but there is no need to panic. Protect the child from sharp, hot, or otherwise dangerous objects. Loosen tight clothing. Do not put anything in the child’s mouth. Do not restrict his/her movements. Roll the child on his/her side and try to keep everyone relaxed.
There are 2 types of febrile seizures: simple and complex. Simple febrile seizures are more common and relatively harmless. They usually last less than 15 minutes and have no after-effects. A neurological examination following a simple seizure will yield no abnormalities.
15. Complex Febrile Seizures
May be more threatening. They can last longer than 15 minutes and although only one side of the body is affected during a complex febrile seizure, neurological reports may indicate abnormalities.
In both cases, febrile seizures pose no threat of mental retardation, cerebral palsy, learning disabilities, or death. Only 25-30% of children who experience one will ever have another. And the incidence of febrile seizures does not indicate a possibility of developing long-term epilepsy. Less than 2% of children who experience febrile seizures will develop epilepsy later in life. Febrile seizures are classed as incidents rather than as a condition.
16. Focal Cortical Dysplasia
This is the most common cause of intractable epilepsy in children and is a frequent cause of epilepsy in adults. All forms of focal cortical dysplasia lead to disorganization of the normal structure of the cerebral cortex.
17. Frontal Lobe Epilepsy
May produce weakness or inability to use certain muscles, including those that govern speech. Frontal lobe seizures may involve thrashing movements during sleep, also stiffening with the head turned to one side and the arm rising into a brief frozen state. Some seizures may be dramatic and upsetting to others, with screaming, bicycling movements of the legs, running. Treatment is with medication, and, in some cases, surgery.
18. Gelastic Seizures
These seizures are both unpredictable and unprovoked by the person’s surroundings. They are abrupt in onset and quickly over. They may occur nocturnally, waking you from sleep and leaving you exhausted. Basically, they are characterized by brief outbursts of emotion, usually in the form of a laugh or a cry. They may be accompanied by forced eye movements, chewing or grinding the teeth, tonic posturing, and clonic jerking. You may appear confused and/or dazed during and after an episode. Gelastic seizures usually last 5 to 60 seconds and you may remember them clearly or may be completely unaware of what occurred.
19. Infantile Spasms (West Syndrome)
These consist of a cluster of sudden jerks followed by stiffening. Often the arms are flung out as the knees are pulled up and the body bends forward.
Infantile spasms consist of clusters of sudden, quick movements. Typically, if the child is sitting up, the head may fall forward, the arms will flex forward, and the body may flex at the waist. If lying down, the knees will be drawn up, with arms and head flexed forward as if the body is reaching for support. Individual spasms last only 1 or 2 seconds. They often repeat in a series of 5 to 50 or more. A child may have many series per day. Spasms are most likely to occur when the child is drowsy, just waking from a nap or falling asleep. They’re sometimes called “jackknife seizures” and are very rare. They occur only during the first year of life, usually starting around 3-7 months of age. Many children with infantile spasms have associated developmental delay and may go on to develop other forms of epilepsy, such as Lennox-Gastaut syndrome.
20. Jacksonian Seizure (Also called Jacksonian March)
A kind of simple partial seizure. “Simple” in this context means patients do not lose awareness. Partial means that abnormal neuron firing only occurs in part of the brain, and, accordingly, abnormal movement or sensation is limited to only part of the body. The characteristic features of Jacksonian march are that it only occurs on one side of the body and it progresses in a predictable pattern from twitching or a tingling sensation or weakness in a finger, a big toe or the corner of the mouth, then marches over a few seconds to the entire hand, foot or facial muscles.
Jacksonian march seizures are generally brief and relatively mild. They are episodic, come and go. There is no confusion afterwards. Sometimes patients may not even notice them. Some patients may also have a phenomenon called “automatism,” such as compulsively licking the lips, fumbling with clothing, or other rhythmic finger movements. Others may experience head turning, eye movement, muscle cramping, numbness, tingling, and a crawling sensation over the skin. Hallucinations can occur too, which can be visual or auditory, meaning patients may see or hear things that are not there.
21. Juvenile Myoclonic Epilepsy
(Also called Janz’s syndrome, impulsive petit mal, myoclonic epilepsy of adolescence, and jerk epilepsy.)Typically begins at puberty in otherwise healthy children. The first symptom is usually a generalized convulsion. These children may also have myoclonic seizures (jerking of the muscles) on awakening. A hand may suddenly fling out, a shoulder may shrug, a foot may kick, or the entire body may jerk. A child may spill or drop whatever he or she is holding or fall from their chair. Absence seizures may also occur. Juvenile myoclonic seizures can occur as a single event or in a series.
22. Lafora Disease
Is a severe form of epilepsy, characterized by seizures and progressive neurological degeneration. It occurs during late childhood or early adolescence. Death usually occurs within 10 years of the first symptoms.
23. Landau-Kleffner Syndrome
Also a rare disorder beginning between ages of 3 and 7. Produces seizures and affects speech. Children develop normal speech, and then slowly lose it. Simple partial and tonic clonic seizures. Treated with antiepileptic drugs to control seizures, and, possibly, steroids.
24. Lennox-Gastaut Syndrome
Affects between 3-10% of children with epilepsy, more commonly males. The peak age for onset is between 1 and 8 years of age with extreme incidence occurring in the first and tenth years of life The most characteristic manifestation of the Lennox-Gastaut syndrome is in a large variety of seizures.
Tonic seizures, the most inherent kind associated with the syndrome, may occur at any time, both day and night. They are usually brief and consciousness is often impaired. Those cases which do appear nocturnally usually occur during the periods of slow-wave sleep in the latter part of the night.
Atypical absence seizures are also present in many cases. Such seizures can begin and end gradually with consciousness only partially affected. The child may continue to be active, however distant or abstracted thoughts. Often, there is a loss of facial and the neck muscles, accompanied by imbalance and abnormal posture. They might lean forward with an open mouth and signs of myoclonic epileptiform activity may become evident in a twitching of your eyelids and mouth. In such cases, massive myoclonic jerks, myoclonic-atonic attacks, as well as atonic seizures may occur, though much less frequent and severe than the other traits.
Tonic-clonic, clonic, or partial seizures are also characteristic of the syndrome and usually are evidence of an underlying cerebral disorder. Even worse, severe cases of status epilepticus may develop, leaving the child unconscious with a continuous array of atonic and myoclonic-atonic seizures. Such seizures may persist through days, weeks, or even months, causing possible mental developmental delay and physical repercussions.
25. Limbic Epilepsy
Limbic areas are regions in the temporal and frontal lobes, which are involved with memory and emotion and this is a seizure happening in this area.
26. Motor Seizures
They are a form of simple partial seizures which include clonic, jerking, convulsive movements. Jerking typically begins in one area of the body – your face, arm, leg, or trunk — and may spread to other parts of the body. These seizures are sometimes called Jacksonian motor seizures, their spread is called a Jacksonian march and they cannot be stopped.
27. Multifocal Seizures
While most seizures can be neatly split into partial and generalized, there exists some that don’t fit. For example: the seizure may be generalized only within one hemisphere. Alternatively there may be many focal points (multifocal seizures) that are distributed in a symmetrical or asymmetrical pattern.
28. Musicogenic Seizures
This reflex epilepsy is triggered by certain types of music or even specific frequencies of pitch for which your brain has a low threshold or tolerance. They usually involve a degree of cognitive or emotional appreciation of the stimulus. This usually results in a complex partial seizure, but may also induce others, such as tonic-clonic seizures. Sensitivity to music varies from person to person. Some people are sensitive to a particular tone from a voice or instrument. Others are sensitive to a particular musical style or rhythm. Still others are sensitive to a range of noises.
29. Neonatal Seizures
Neonatal seizures occur in babies soon after birth. As many as 1.5 to 2.5% of newborns have seizures in the first month of life. A further 20% of all seizures in children under 3 years of age have neonatal seizures. They’re generally classified as subtle, clonic, tonic, and myoclonic.
Subtle attacks are characterized by apneas with episodes of pallor, fixed staring, deviation of one or both eyes, eye blink, motor changes, episodic chewing movements, or stereotypic limb movements such as swimming or bicycling motions. Drooling and unusual alertness may accompany neonatal seizures. Usually, most neonatal seizures occur over only a few days and fewer than half of affected infants develop seizures later in life.
30. Nocturnal Seizures
These are usually tonic-clonic. They might occur just after a person has fallen asleep, just before waking, during daytime sleep, or while in a state of drowsiness. People who experience nocturnal seizures may find it difficult to wake up or to stay awake. Although unaware of having had a seizure while asleep, they may arise with a headache, have temper tantrums, or other destructive behavior throughout the day.
Nocturnal seizures are very uncommon and their mechanisms poorly understood. There is evidence that sleep enhances epileptic discharges in the EEG, though their daytime recordings may appear to be normal. However, if a pattern of limiting seizures to the hours of slumber is maintained, the chance of them occurring during the daytime is greatly reduced.
31. Partial (Focal) Seizure
They may occur at any age, as a single episode or as a repeated, chronic seizure disorder. They are seen less frequently in children than in adults, but still account for about 45% of pediatric seizure disorders. Patients with focal seizures can have any of the symptoms below. Those with simple focal seizures do not lose consciousness and will be aware and remember the events that occur at the time. If you have complex partial seizures, you will have abnormal consciousness and may or may not remember any or all of the symptoms or events surrounding the seizure.
Symptoms include: abnormal muscle contractions affecting one side of the body, abnormal head movements, staring spells, abnormal mouth movements like lip smacking, chewing or swallowing without cause, numbness, tingling, abdominal pain, nausea, or discomfort, sweating, a flushed face, rapid heart rate or pulse, sensation of déjà vu and changes in mood or emotion. (That about covers everything, doesn’t it?)
32. Pattern — Sensitive Epilepsies
In this reflex condition, seizures are produced by particular visual patterns. These triggers may consist of circles, stripes, or other patterns, usually of high contrast. Moving patterns are most likely to incite a seizure.
33. Photosensitive Epilepsy
If you have photosensitive epilepsy, certain types of flickering or flashing light may incite a seizure. The trigger could be exposure to television screens due to the flicker or rolling images, computer monitors, certain video games or TV broadcasts containing rapid flashes, even alternating patterns of different colors, in addition to intense strobe lights. And surprisingly, seizures may be triggered by natural light, such as sunlight, especially when shimmering off water, even sun flickering through trees or through the slats of Venetian blinds.
34. Post Traumatic Seizures
Seizures may develop immediately after an injury to the brain or may develop in delayed fashion, showing up months or years after the initial trauma. Generally speaking, the risk of post traumatic seizures is related to the severity of the injury. The greater the injury, the higher the risk of developing seizures. Even mild to moderate injuries can result in seizures.
It is thought that a head injury disrupts the pathways of the brain and that an epileptic seizure can be viewed as a sort of short circuit of the brain’s electrical functioning. During the seizure the electrical fields in the brain are overloaded, resulting in seizures. The most commonly seen seizures related to traumatic brain injury are “generalized” seizures, which are also called tonic-clonic or “grand mal” seizures.
35. Primary Reading Epilepsy
This is a reflex epilepsy where seizures are triggered by reading. Seizures usually begin in adolescence, and onset is unusual in younger children or adults over 30 years old. Patients report jaw jerking or clicking while reading, often with jerks of the arms, and if reading continues, a generalized convulsion may occur. Transient cognitive impairment has also been noted with the jerks.
36. Progressive Myoclonic Epilepsy
A rare, form of epilepsy with myoclonic (jerking) and tonic-clonic (grand mal) seizures. Children with this condition may have trouble with maintaining balance and experience rigid muscles. There is also a loss of mental ability. A gene for this disorder has recently been discovered
37. Psychogenic Seizures (PNES or “Pseudo Seizures”)
Psychogenic seizures are not classified as a form of epilepsy. They may be brought on by stress, trauma, anxiety or a history of sexual abuse.
It’s difficult to differentiate between psychogenic and epileptic seizures. However, one reliable indicator of a psychogenic seizure is eye closure during the seizure. If you have a seizure, your eyes tend to stay open. Still, statistics indicate that, in 20-30% of cases, epileptologists are incorrect in attempting to distinguish one from the other. Although psychogenic seizures are not caused by electrical discharges in the brain and thus do not register any EEG abnormalities, they are often mistaken for epileptic disorders. It’s also possible to have both psychogenic seizures and epilepsy. Most patients with psychogenic seizures are misdiagnosed and consequently treated with epilepsy drugs or other epilepsy therapies, sometimes with severe and fatal side effects.
38. Rasmussen’s Encephalitis — also Chronic Focal Encephalitis (CFE)
This is a rare, progressive neurological disorder which affects one half of the brain, producing severe seizures, loss of motor control and speech along with paralysis on one side of the body. Various treatments have been tried, including surgery to remove the affected half of the brain.
39. Reflex Epilepsy
A seizure is considered a reflex seizure when it occurs as a direct response to a particular stimulus or event in the environment. These seizures are experienced by approximately 6% of people with epilepsy. They can be triggered by visual stimulation, a sudden “startle”, or a variety of other factors alone or in combination. If a patient only has seizures as a result of a certain stimulus then it is possible to control them by avoidance. Begins in childhood, is associated with absence epilepsy, and may disappear in adulthood.
40. Secondarily Generalized Seizures
Generally, they’re partial seizures evolving into generalized seizures, most often with tonic-clonic convulsions. The partial seizures which were once limited to one hemisphere of the brain progress to encompass the entire brain bilaterally, causing a generalized seizure. The clinical nature of a secondarily generalized seizure usually does not differ from that of the initial, originating seizure.
Secondarily generalized seizures are predominant in 16% of all children and 9% of all adults with seizure disorders. Most people with complex partial seizures and many with simple partial seizures will experience such a seizure at some point. When they occur frequently, the chances for future partial seizures may be increased.
41. Simple Partial Seizures (Focal Seizures)
Although your ability to respond may be preserved, motor manifestations or anxiety relating to the seizure symptoms may prevent you from responding appropriately You may see or hear things that are not there. Feel emotions, often fear, but sometimes sadness, anger, or joy. There may be a bad smell or a bad taste, a funny feeling in the pit of your stomach or a choking sensation. Sudden or restless movement or vision distortion are also characteristics. These seizures are sometimes called simple partial seizures of temporal lobe origin or temporal lobe auras.
42. Sensory Seizures
Some simple partial seizures consist of a sensory experience. People with sensor seizures may smell or taste things that aren’t there, hear clicking, ringing, or a person’s voice when there is no actual sound. You may also see lights, hear a buzzing sound, or feel tingling or numbness in a part of the body. Simple partial seizures usually last just a few seconds, although they may be longer. If there are no convulsions, they may not be obvious to those around you.
43. Startle Epilepsy
This is a type of reflex epilepsy in which seizures are provoked by loud noises or sudden surprises. Most patients with startle epilepsy are only sensitive to one sensory modality (i.e. temperature, taste, sound, pressure); however, it is the unexpected nature of the stimulus, rather than the sensory modality, that characterizes startle epilepsy. These seizures usually last less than 30 seconds. The seizure begins with a startle response, followed by a brief tonic phase. Patients sometimes fall to the ground and experience clonic jerks. Responsiveness to the stimulus decreases as a result of repeated exposure to the stimulus. Spontaneous seizures also occur in patients with startle epilepsy, but are infrequent in most cases.
People with startle epilepsy usually have static cerebral lesions and developmental delay. For many people, half of the body is partially paralyzed and it is the weak side of the body that is primarily involved in the startle seizures. Startle epilepsy is often associated with disorders such as Down syndrome and cortical dysplastic lesions.
44. Status Epilepticus
Status epilepticus (SE) is a common, life-threatening neurologic disorder. It is essentially an acute, prolonged epileptic crisis. Aggressive treatment is necessary. Maintenance of vital signs, including respiratory function, is of major importance. It may occur as a first seizure or if you are known to have seizures. Duration may last for a long time, or repeat without recovery. This prolonged or repeated seizure activity can result in death if it’s not treated immediately. Status epilepticus can be convulsive (tonic-clonic or myoclonic seizures) or non-convulsive (absence or complex partial seizures). A person in non-convulsive status epilepticus may appear confused or dazed.
45. Temporal Lobe Epilepsy
The seizures associated with temporal lobe epilepsy consist of simple partial seizures without loss of awareness and complex partial seizures, with loss of awareness. You lose awareness during a complex partial seizure because the seizure spreads to involve both temporal lobes, which causes impairment of memory. The result is complex partial seizures coupled with simple partial seizures. Generalized tonic clonic seizures may be part of this syndrome as well.
46. Tonic Seizures
Tonic seizures are characterized by facial and muscle spasms of your trunk, flexing or reaching of your upper and lower extremities, and impaired consciousness. Several types of tonic seizures exist. Those grouped with absence, myoclonic, and atonic seizures are non-convulsive and tend to be brief. The more prolonged seizures usually are convulsive and may manifest dilation of your pupils, tachycardia, apnea, a bluish tinge to your skin, salivation, and the loss of bladder or bowel control. Tonic seizures are often followed by postictal confusion.
47. Tonic-Clonic Seizures (“Grand Mal”)
In a generalized tonic-clonic (grand mal) seizure, you will probably give out a short cry and fall to the floor. Your muscles will stiffen during the tonic phase and then, during the clonic phase your extremities will jerk and twitch. Often you will lose consciousness, stop breathing or have difficulty breathing, turn blue and lose bladder control which in not uncommon, but extremely embarrassing.
Afterwards, you may feel tired, confused and disoriented. This may last from 5 minutes to several hours or even days. Rarely, this disorientation may last up to 2 weeks. You may asleep, or gradually become less confused until full consciousness is regained.
48. Vertigo Epilepsy
While epilepsy is commonly accompanied by dizziness or vertigo, vertigo is only rarely caused by epilepsy. This arises primarily because vertigo is much more commonly caused by ear conditions. Epileptic vertigo is due to brain injury, typically the part of the temporal lobe that processes vestibular signals. Loss of consciousness usually occurs at the time of injury. The typical symptom is “quick spins.”
49. Withdrawal Seizures
This type of seizure is seen when certain medications, such as barbiturates and benzodiazepines, are stopped abruptly. In this case, continued treatment with antiepileptic medications is usually not advisable. Withdrawal seizures are common when a person with alcoholism is trying to quit drinking. If a person with epilepsy drinks alcohol heavily and experiences withdrawal seizures, it is difficult for the physician or specialist to determine the exact cause of the seizure and to determine the next appropriate step. Therefore, it is important to avoid alcoholic beverages once you begin taking antiepileptic medications.
Credit: epilepsytalk.com for compiling this list.
The lack of sleep, and missed doses of medications, are common causes of increased seizure frequency. It is important to get good quality sleep, between 7-8 hours per night, although some people can thrive on fewer hours.
If going to sleep is a problem, then a having a bedtime routine could be helpful to you such as going to bed at a regular time each night, not drinking alcohol or caffeine beforehand, not eating too late, turning off all your computer/phone/ipad gadgets much earlier and perhaps taking a warm shower before falling into a comfortable bed in a dark room, devoid of distractions and noise.
Having seizures at night can make people sleep deprived, as can sleep disorders and side-effects of some medications. Please consult your GP for help if you are not able to get regular good sleep.
Despite the ills of smoking tobacco (including the possibility of SUDEP) and the proven likelihood of developing smoking-related illnesses (such as strokes, cancer, emphysema and heart attacks), many people with epilepsy use smoking as a stress reliever.
New Zealand is increasingly becoming a smoke-free environment, and there are Quit Smoking programmes available to try, but a conversation with your GP is important in choosing the right programme for you.
Need medical attention after hours?
The South Waikato GP Clinics operate a combined after hours’ clinic from 5 – 6pm weekdays and 10 – 4pm on Saturdays and public holidays. The clinic times and locations are:
Monday: Tokoroa Family Health, Gate 3, Tokoroa Hospital
Tuesday: Putaruru-Tirau Family Doctors, Duke Street, Putaruru, Phone (07) 883 3965
Wednesday: Tokoroa Medical Centre, Gate 3, Tokoroa Hospital
Thursday: Tokoroa Medical Centre, Gate 3, Tokoroa Hospital
Friday: Clinic will be at the practice that is rostered on for the Saturday
Saturday: 10am to 4pm: GP Fast-track clinic, Tokoroa Hospital ED, Gate 1, Tokoroa Hospital
The cost of an after-hours consultation is free for under 13’s, and $35 for adults
Outside of these clinic times, you still have many options:
- Phone your practice or call (07) 886 6111 and your call will be transferred to a registered nurse who can provide assessment and advice
- Visit your local Pharmacist who is trained health professional and can provide treatment for a variety of conditions
- Call Healthline on 0800 611 116 for advice
Please remember that the Emergency Department should only be used for emergencies.
Click here to see the Starship hospital caregivers guide to administering Buccal Midazolam.
What are they? Visit the page below for more information.
Is the patron saint of epilepsy.
A small number of people develop epilepsy after a stroke.
Know the signs and symptoms of a stroke:

For more information visit www.stroke.org.nz or contact the Stroke Foundation on 0800 787 653.
Is a rare and unwitnessed event of someone dying during, or after, a seizure, where no other cause of death can be found. The exact cause of death is not known but a person with epilepsy may have had difficulties with breathing or heart problems, or a combination of both.
A known risk factor of dying of SUDEP is having uncontrolled or poorly controlled seizures, especially convulsive ones. To minimise the risk of dying of SUDEP it would be advisable to take your anti-epileptic medications routinely every day, being vigilant around seizure triggers, and recording all your seizures in a seizure diary so that regular health and medication assessments can be made of your condition.
Using a seizure mattress alarm and anti-suffocation pillows may help, since SUDEP generally happens during sleep.
The findings from studies vary, but statistics suggest that up to 21% of early deaths among people with epilepsy are caused by suicide. This would, of course, significantly influence average epilepsy life expectancy statistics.
This benefit is for people who have, or are caring for someone with a health condition. This benefit is adjusted according to your or your spouse/partner’s income. To qualify you must be aged 16 years or over and unable to regularly work 15 hours or more a week because of a sickness, injury or disability which is expected to last at least two years.
The Supported Living Benefit (SLB) also includes carers of people needing hospital level (or equivalent) care. To qualify, you must be the primary carer for someone at home who would otherwise need the same care at a hospital, rest home, residential disability care, extended services for the elderly or severely disabled, or care of a similar kind. Once again, the SLB is adjusted according to your or your spouse/partner’s income.
If a person’s seizures are a symptom of another condition, then they have a higher risk of mortality (death). People whose seizures begin following a stroke, because of a serious head injury, and particularly because of brain tumors, have a lower life expectancy.
is a group of signs and symptoms that, when added together, suggest a particular medical condition. An epilepsy syndrome has seizures as the central symptom but also includes other features such as specific EEG readings and age dependency.
Here is a useful webpage detailing all of the epilepsy syndromes:
https://www.epilepsy.org.uk/info/syndromes/aicardi-syndrome
See fact sheet 21 on being a teenager and having epilepsy
The Code of Health and Disability Services Consumers’ Rights (0800 11 22 33)
Means that you should have:
- respect and privacy
- fair treatment
- dignity and
- independence
- appropriate standards
- effective communication
- information choice and consent support
- rights during teaching and research
- your complaints taken seriously
Is a subsidised taxi service using vouchers or electronic cards that gives 50% on normal taxi fares. To find out if you are eligible to receive these taxi vouchers please contact: maria@ewct.org.nz.
For more information visit busit.co.nz
- National Transport Assistance, through MOH
www.health.govt.nz/new-zealand-health-system/claims-provider-payments-and-entitlements/national-travel-assistance - Total Mobility Scheme
- Mobility Parking Permit Scheme: www.ccsdisabilityaction.org.nz/mobility-parking/
- Conveyance Allowance through MOE
https://parents.education.govt.nz/learning-support/learning-support-needs/transport-assistance/
https://parents.education.govt.nz/primary-school/your-child-at-school/school-transport-assistance/ -
Within the Waikato Region, people with an impairment that prevents them from being able to drive may be eligible for an Accessibility Concession card.For further information, please follow this link:
Can also be known an ‘intractable’, ‘refractory’ or ‘drug resistant’ epilepsy and it severely interferes with the quality of life for those living with the condition. For those deemed to have uncontrolled epilepsy, questions would be asked around the epilepsy diagnosis, treatment and life style of the person. Good communication with a trusted neurologist is important in gaining a long-term solution to a difficult problem.
Should be discussed with your GP and/or epilepsy specialist.
Is a small, electrical device, similar to a pacemaker, which is placed in a person’s chest under general anaesthetic. A thin wire runs from the device to the vagus nerve and sends out electrical impulses at regular intervals to reduce the severity of seizures, or even stop them, although the exact mechanism through which it reduces seizures is still not completely clear.
See this PDF for more information.
Why Video Seizures?
Doctors often don’t see their patients’ seizures because they may not happen during appointments (unless you go to an EMU). So, doctors often have to make a diagnosis based on other people’s descriptions of what happens (plus using EEG’s and other techniques). But if they can watch a seizure video, it can make their job a lot easier.
Providing videos of your seizures to your neurologist or treatment team can be really useful for a few different reasons:
- Seizure videos are especially useful during a new diagnosis. They help your doctor work out which kinds of seizures you’re having, and can give clues about where in your brain they begin. Videos are also useful for ongoing care.
- If the type, frequency or severity of seizures change, then having video available is very helpful.
- If you have most seizures at night, your doctor may never be able to see your seizures for themselves. So a nocturnal seizures video, recorded using a special night time camera, could be helpful. It’s possible to buy night time cameras online – they’re often fairly cheap according to this article on Medium.
- Seizure videos are also useful for helping with misdiagnosis – good quality footage can help epileptologists tell if someone actually has epilepsy, non-epileptic seizures, or a different condition.
If you remain conscious during your seizures, you might be able to record a video of these events yourself, using the ‘selfie’ mode on your smartphone. For most people, recording videos of their own seizures isn’t possible. If that’s the case for you, then speak with friends, family, teachers and other people you spend time with about making recordings of your seizures on their smartphones.
Vidoeing tips:
Safety first: Making sure the person who’s having a seizure is safe is ALWAYS the priority. If they have fallen over, attend to them and ensure they are in a safe position and away from any harm. Only once you’re sure they are in a safe position should you record a video of a seizure.
Try to capture the start of the seizure: The first few seconds of a seizure can provide a lot of information about where in the person’s brain the seizure begins. Seizures are usually hard to predict, but if the person has an aura or can tell when their seizures are coming on, start filming as soon as it’s safe to do so.
Record their whole body: As far as possible, try to capture the person’s whole body during your recording (rather than just their face). There are lots of subtle movements the person might make which are helpful to doctors.
Record noises too: The noises a person makes during a seizure can also be helpful – try your best to capture words and sounds they make.
Film until the person returns to consciousness: If possible, try to record the entire seizure, until the person has returned to consciousness. You can check how ‘aware’ they are by asking simple questions (such as: ‘what day of the week is it?’).
Ethics and seizure videos:
For many people, seizures are a highly personal and private experience. So, although recording a video of them can be helpful, there are numerous ethical issues to be aware of. In the ideal scenario, the person with epilepsy will have told you in advance that they’re happy for you to record videos of their seizures.
Either way, you must always inform them that you recorded a video once they recover.
A couple of other rules: It should go without saying, but DO NOT post videos of anyone’s epileptic seizures on social media – especially if they haven’t given you permission.
You should not share the video with anyone else without the person’s permission. You should send a copy of the video of the seizure to the person with epilepsy (or their carer). Normally, you should delete the video after sending it to them, unless the person has said you can keep it
Do not expect the person who has epilepsy to want to watch your seizure video – they might find it frightening, embarrassing or uncomfortable If the person who had the seizure is a child or does not have the intellectual capacity to give informed consent, then you must share the video with that person’s parents or carer. You should still try to tell them you have made a recording in a way they can understand.
A person of any age, can develop epilepsy regardless of their IQ, ethnicity, and social standing. Epilepsy is commonly found in children, under the age of two years, and the elderly over the age of 65 years old. Around 1 in 100 people have epilepsy, which is about 43,000 New Zealanders and about 70 million people globally.
Is a form of electromagnetic radiation widely used in medicine and science. Medical uses include the widely known radiographs (classic 2-dimensional X-ray images) and computed tomography (CT) scans (cross sections or ‘slices’ converted to 3 dimensional images).
is available to you on request. Ask your GP.
New Zealand Government Zero Data Scheme. Essentially if you have a phone capable of connecting to the internet but have no data, use the site below to access the host of Governtment services listed without having to pay for the data.
“Zero Data is available to anyone using a mobile device connected to the Spark, Skinny, One NZ, 2degrees, Warehouse Mobile, Slingshot or Orcon mobile networks.
Use this site to get free access to the websites listed below from your mobile – you don’t need data but you do need it turned on.”
https://zero.govt.nz/ NZ Govt Zero Data Portal
For all children under the age of 13 years to see a GP in New Zealand. See health.govt.nz for more information.